 
We hypothesize that the concurrent use of DOACs plus ASA in individuals with AF or AFL will result in lower rates of MACE when compared to DOAC use alone. Therefore, there is inconclusive evidence to guide physicians on when to continue or to add ASA therapy in patients with AF/AFL using DOACs. The most recent 2016 European Society of Cardiology guidelines emphasize that the use of combination OAC with antiplatelets is contraindicated because of harm (Class III) as this increases bleeding risk and should be avoided in AF patients without another indication for antiplatelet therapy. The 2014 American Heart Association/American College of Cardiology/Heart Rhythm Society practice guidelines and its 2019 focused update for the management of AF do not provide any specific recommendation on concurrent DOAC+ASA use for primary or secondary prevention. Apart from acute coronary syndrome (ACS) and percutaneous coronary or vascular interventions, there is no clear, evidence-based threshold to continue or add ASA for primary or secondary prevention of major adverse cardiovascular events (MACE) in the setting of AF or AFL treated with OAC. Before patients are diagnosed with AF or AFL, a significant number of them already take aspirin (ASA) for either primary or secondary prevention of cardiovascular disease. OAC can be accomplished with the vitamin K antagonist (VKA) warfarin or one of the direct oral anticoagulants (DOACs) apixaban, edoxaban, dabigatran, or rivaroxaban. Oral anticoagulation (OAC) based on stroke risk stratification with CHA2DS2-VASc scores has been the mainstay of stroke prevention therapy. 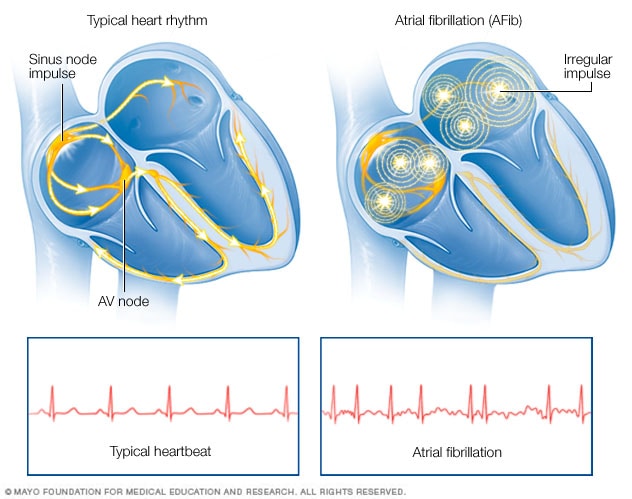
ORBIT-AF demonstrated that 31% of patients with AF had one or more hospitalizations per year. In the Framingham Heart Study cohort, AF was associated with an increase in the risk of mortality to a 1.5-fold in men and 1.9-fold in women. AF and AFL are independently associated with increased mortality and morbidity, including stroke, cardiomyopathy, frequent hospitalizations, and cognitive decline. Atrial flutter (AFL) is less common, with an estimated incidence of 200,000 cases per year in the United States. These findings underscore the potential harm of this combination therapy when used without a clear indication.Ītrial fibrillation (AF) is the most common cardiac arrhythmia, with a prevalence of 1% in the United States. In this observational analysis of patients with atrial fibrillation and flutter, the concomitant use of direct oral anticoagulants and aspirin was associated with an increased risk of both major adverse cardiac and bleeding events when compared to the use of direct oral anticoagulants alone. The rate of death was not statistically different between the groups, (HR 0.87, 95% CI (0.61–1.25)). The rate of bleeding was also higher in the exposed group, (HR 1.30, 95% CI (1.11–1.52)). After using propensity scores to balance the baseline characteristics in both groups, the analysis revealed higher rate of major adverse cardiac events in the exposed group compared to the unexposed group, (HR 2.11, 95% CI (1.74–2.56)) with a number needed to harm of 11 (95% CI ). The group exposed to aspirin contained 2908 subjects, and the group unexposed to aspirin contained 3096 subjects. 
Six thousand four patients were in the final analysis, 57% males and 80% Caucasians, median age 71, interquartile range (63–80). Secondary outcomes were bleeding and death. Primary outcome was major adverse cardiac events, defined as acute coronary syndromes, ischemic strokes, and embolic events. Patients were classified into two groups based on concurrent aspirin use and observed for a minimum of 2 years. Exclusions were history of venous thromboembolic disease and use of other antiplatelet therapies such as P2Y12 inhibitors. Retrospective study of adult patients between 18 and 100 years old who have nonvalvular atrial fibrillation or flutter and were started on a direct oral anticoagulant (apixaban, rivaroxaban, or dabigatran), between Januand Septemwithin the Beaumont Health System. We aimed to assess whether concurrent aspirin and direct oral anticoagulant therapy for atrial fibrillation or flutter will result in less coronary, cerebrovascular and systemic ischemic events compared to direct oral anticoagulant therapy alone. The benefit of combining aspirin and direct oral anticoagulants on the reduction of cardiovascular events in atrial fibrillation or flutter is not well studied.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
